
Some health issues are hard to talk about, even with your health care provider, but it’s important that you do. One such condition is hemorrhoids. An estimated 1 in 20 Americans have symptomatic hemorrhoids. They affect people of all ages, genders, races and ethnicities. They’re more common as you age, affecting more than half of people over age 50. Women are more likely to get hemorrhoids while pregnant. Hemorrhoids can also occur after cases of chronic diarrhea.
Physician Tip: Hemorrhoids and anal fissures cause similar symptoms, such as itching, pain and bleeding. While swollen veins cause hemorrhoids, a tear in the lining of the anus causes an anal fissure. Your health care provider will do a physical exam and may order tests to find what’s causing your symptoms.
Types of Hemorrhoids:
Hemorrhoids can happen inside or outside the rectum. The type depends on where the swollen vein develops. Types include:
- External: Swollen veins form underneath the skin around the anus. Your anus is the canal where poop comes out. External hemorrhoids can be itchy and painful, but they typically do not bleed. Sometimes clots can occur. This is not dangerous, but can result in pain and swelling.
- Internal: Swollen veins form inside the rectum. Your rectum is the part of the digestive system that connects the colon (large intestine) to the anus. Internal hemorrhoids may bleed, but they usually aren’t painful.
- Prolapsed: Internal hemorrhoids can prolapse, meaning they stretch and bulge outside of the anus. These hemorrhoids may bleed or cause pain.
What can I do to prevent Hemorrhoids from becoming a problem?
- Increase fiber in your diet and drink more water. Eat more high-fiber foods (fresh fruits, vegetables and whole grains) or take supplements to fill in any gaps in your diet. Generally, women should aim for 25 grams of fiber per day, while men should get 35 grams of fiber. Check out our fiber recommendations.
- Avoid foods that often cause constipation, such as white rice, white bread and other processed grains, red meat, alcoholic beverages and bananas. This will help your stool move through your digestive system with less straining.
- Avoid pushing or straining excessively during bowel movement. If constipation occurs often, incorporate more water, fiber and try a “squatty potty” for help with proper alignment for a bowel movement (more about this in tip #7).
- Go to the toilet when the urge hits — don’t delay bowel movements.
- Stay physically active. Being on the move keeps bowels moving.
- Maintain a healthy body weight. Being overweight significantly raises the risk of having hemorrhoids.
- Squatting to poop is a more natural position than sitting. Squatting relaxes your puborectalis muscle more and straightens out your colon, giving the bowel movement a straight route out.
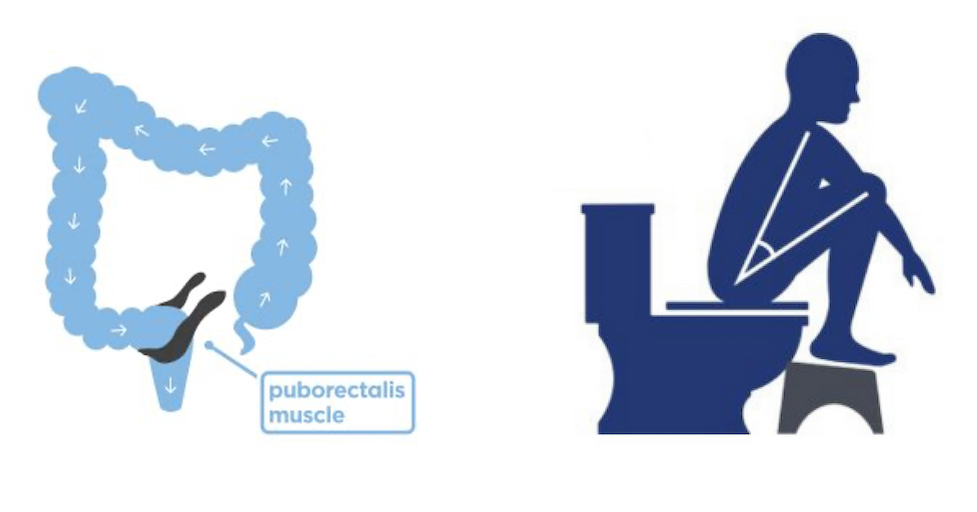
Physician Tip: Squatty Potty, a stool that raises your knees above your hips to put you into a squat-like position when you poop.

Symptoms often improve with at-home treatments, but on occasion people need medical procedures. For symptoms in which you need to seek medical assistance, click here.
What can I do at home to help ease hemorrhoid symptoms?
Home remedies can help with the associated pain and itching of hemorrhoids as well. Soaking in a warm sitz bath a few times a day often eases symptoms. Pain relievers and anti-itch creams may also be recommended.
- Take a sitz bath. Fill a bathtub with four to six inches of warm water. You may also use a sitz bath pan that fits inside a toilet bowl. Sit in the sitz bath for 15 minutes. Do this three times a day, and after each bowel movement. The warm water can help decrease pain and swelling.
- Use toilet paper with lotion or flushable wet wipes to gently pat and clean your bottom after pooping.
- Apply over-the-counter medications: Desitin and other diaper rash creams work best.
- Soften stool by taking laxatives (Consult your physician before taking laxatives)
- Some painkillers — such as aspirin, ibuprofen and acetaminophen — may alleviate the pain and discomfort. (Consult your physician before taking such medications for pain)
If you are experiencing symptoms of hemorrhoids such as rectal bleeding or blood in your stool, always consult with a physician, as bleeding can be a sign of other serious conditions. Seek the advice of a physician before trying any treatment options.
How are hemorrhoids diagnosed?
Your health care provider diagnoses hemorrhoids based on symptoms and a physical exam. You may also have:
- Digital rectal exam: Your provider inserts a gloved, lubricated finger into the rectum to feel for swollen veins.
- Anoscopy: Your provider uses an anoscope (lighted tube) to view the lining of the anus and rectum.
- Sigmoidoscopy: Your provider uses a sigmoidoscope (lighted tube with a camera) to view inside the lower (sigmoid) part of the colon and rectum. Procedure types include flexible sigmoidoscopy and rigid sigmoidoscopy (proctoscopy).
These tests may be uncomfortable but aren’t painful. They typically take place in a doctor’s office or outpatient center without anesthesia. You go home the same day.
If you have questions about treatments and surgery for persistent hemorrhoids, our colorectal expert, Erik Grossmann, MD, answers your questions and helps you prepare for your surgery here.
To Make an Appointment
Your initial consultation gives you the opportunity to meet our team, learn more about our services and find out which treatment options will best meet your needs. To schedule a prompt appointment with Dr. Erik Grossmann, please call Columbia Surgical Associates at 573-443-8773.


Leave a Reply